Canine Cardiopulmonary Arrest Study Guide
Canine Cardiopulmonary Arrest
NAVLE Study Guide
Cardiovascular System | Species: Canine
Estimated Read Time: 35-40 minutes | Last Updated: December 2024
Overview and Clinical Importance
Cardiopulmonary arrest (CPA) is the sudden cessation of effective cardiac and respiratory function, resulting in loss of consciousness and the absence of a palpable pulse. This life-threatening emergency requires immediate intervention through cardiopulmonary resuscitation (CPR) to restore circulation and oxygenation. Understanding the pathophysiology, recognition, and evidence-based management of CPA is essential for the NAVLE, as it represents one of the most critical emergency scenarios encountered in veterinary practice.
Despite advances in veterinary medicine, survival to discharge after CPA remains low, with only 5 to 7 percent of dogs surviving to hospital discharge. However, dogs experiencing CPA during anesthesia have significantly better outcomes, with up to 17 times higher survival rates when CPR is initiated promptly. The 2024 RECOVER (Reassessment Campaign on Veterinary Resuscitation) guidelines provide the current evidence-based framework for CPR in dogs and cats.
Please look at RECOVER CPR Algorithm for Dogs and Cats
Learning Objectives
- Define cardiopulmonary arrest and differentiate it from respiratory arrest
- Identify common causes and risk factors for CPA in dogs
- Recognize clinical signs indicating CPA and determine when CPR is indicated
- Perform Basic Life Support (BLS) according to RECOVER 2024 guidelines
- Implement Advanced Life Support (ALS) including drug therapy and defibrillation
- Understand post-cardiac arrest care and factors affecting prognosis
Etiology and Pathophysiology
Common Causes of Cardiopulmonary Arrest
Cardiopulmonary arrest in dogs is typically multifactorial and can result from numerous underlying conditions. Unlike humans, where coronary artery disease is the predominant cause, CPA in dogs more commonly results from progressive systemic illness, trauma, or anesthetic complications.
| Category | Common Causes |
|---|---|
| Cardiac | Dilated cardiomyopathy (DCM), arrhythmogenic right ventricular cardiomyopathy (ARVC), severe arrhythmias (ventricular fibrillation, asystole), pericardial effusion with tamponade, myxomatous mitral valve disease with acute rupture |
| Respiratory | Severe pneumonia, pulmonary thromboembolism, airway obstruction, pleural effusion, pneumothorax, drowning, aspiration |
| Anesthetic | Anesthetic overdose, vagal reflex, hypotension, hypoxemia, hypoventilation, malignant hyperthermia |
| Trauma | Blunt force trauma, hemorrhage, tension pneumothorax, diaphragmatic hernia, head trauma |
| Metabolic/Systemic | Severe electrolyte abnormalities (hyperkalemia, hypocalcemia), septic shock, hypovolemic shock, gastric dilatation-volvulus (GDV), severe hypoglycemia, hypothermia |
| Toxicologic | Cardiotoxins (digitalis, calcium channel blockers, beta-blockers), respiratory depressants (opioids, barbiturates), organophosphates |
High-Yield Note: On the NAVLE, remember that dogs experiencing CPA during anesthesia have a 17 times higher survival rate compared to non-anesthetic causes. This is because immediate intervention is available and reversible causes (vagal stimulation, drug overdose) can be quickly addressed.
Pathophysiologic Mechanisms
Cardiopulmonary arrest results in immediate cessation of blood flow and oxygen delivery to vital organs. The pathophysiologic cascade includes:
- Global tissue ischemia: Within seconds of CPA, cerebral blood flow ceases, leading to loss of consciousness. Brain cells begin to die within 4 to 6 minutes without oxygen.
- Metabolic acidosis: Anaerobic metabolism leads to lactate accumulation and severe acidemia. Normal lactate is less than 2 mmol per L; levels often exceed 10 mmol per L during CPA.
- Sympathetic response: Initial intense sympathetic stimulation causes peripheral vasoconstriction, but the vasomotor center fails after 10 to 15 minutes without perfusion.
- Post-cardiac arrest syndrome: Even after return of spontaneous circulation (ROSC), multiorgan dysfunction persists, including myocardial stunning, systemic inflammatory response, and reperfusion injury.
Cardiac Arrest Rhythms
The terminal cardiac rhythm present during CPA determines treatment strategy. In veterinary medicine, approximately 61 percent of dogs present with non-shockable rhythms.
| Rhythm | ECG Characteristics | Treatment Approach |
|---|---|---|
| Asystole | Flat line with no electrical activity. Most common terminal rhythm in small animals. | NON-SHOCKABLE: Continue CPR, administer epinephrine every 3-5 minutes, single dose atropine may be considered |
| Pulseless Electrical Activity (PEA) | Organized electrical complexes at rate less than 200 per minute but no palpable pulse | NON-SHOCKABLE: Continue CPR, treat underlying cause (hypovolemia, tension pneumothorax, tamponade), epinephrine |
| Ventricular Fibrillation (VF) | Chaotic, disorganized ventricular activity with no effective contractions. Irregular waveforms of varying amplitude. | SHOCKABLE: Defibrillation is priority. If less than 4 minutes duration, defibrillate immediately. If greater than 4 minutes, perform 2-minute BLS cycle first, then defibrillate. |
| Pulseless Ventricular Tachycardia | Wide, bizarre QRS complexes at rate greater than or equal to 200 per minute without pulse | SHOCKABLE: Treat same as VF - defibrillation indicated |
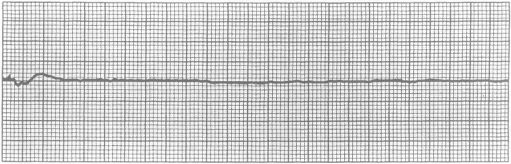
(Figure 1) - ECG tracings showing asystole, PEA, ventricular fibrillation, and pulseless VT
Memory Tip - SHOCK vs NO-SHOCK Rhythms: SHOCK the 'V's: VF and VT (pulseless) NO-SHOCK: Asystole and PEA Remember: 'VF and VT get electricity, Asystole and PEA get chemistry (drugs)'
Recognition and Diagnosis of Cardiopulmonary Arrest
Clinical Signs
Rapid recognition of CPA is critical for survival. The 2024 RECOVER guidelines emphasize that CPR should be initiated within 10 to 15 seconds of recognizing CPA.
Primary signs of CPA:
- Unresponsiveness: No response to verbal or physical stimulation
- Absent or agonal breathing: No chest wall movement or irregular gasping breaths
- No palpable pulse: However, pulse palpation is unreliable and should NOT delay CPR initiation
- Dilated pupils: May occur but is not required for diagnosis
- Cyanotic or pale mucous membranes: Poor tissue perfusion
Board Tip: The 2024 RECOVER guidelines specifically state that pulse palpation is NOT recommended for diagnosing CPA because it is unreliable and delays CPR. If a dog is unresponsive and not breathing (or only showing agonal gasps), START CPR immediately without checking for a pulse. This is a testable concept on the NAVLE.
Initial Assessment Algorithm
The RECOVER CPR Initial Assessment Algorithm provides a systematic approach to CPA recognition:
- Stimulate: Shake and shout to assess responsiveness
- Check breathing: Look for chest wall movement
- If not breathing or only agonal gasps: Call for help and begin CPR
- Do NOT: Waste time checking pulse or performing extensive diagnostics
Basic Life Support (BLS)
Basic Life Support consists of chest compressions and ventilation to maintain minimal blood flow and oxygenation until advanced interventions can be implemented. The 2024 RECOVER guidelines include several important updates to BLS techniques.
Chest Compressions
High-quality, uninterrupted chest compressions are the cornerstone of successful CPR. Even ideal compressions only achieve approximately 30 percent of normal cardiac output.
| Patient Type | Position and Technique | Compression Depth |
|---|---|---|
| Small Dogs and Cats (under 10 kg) | LATERAL recumbency. Three technique options: 1. Circumferential two-thumb technique: Both thumbs over heart 2. One-handed technique: Thumb on one side, fingers on other 3. Heel of hand technique | One-third to one-half of chest width |
| Medium to Giant Dogs (over 10 kg) | LATERAL recumbency. Hands interlocked over widest part of chest. Rescuer shoulders directly above hands, elbows locked, using core muscles for compressions. | One-third to one-half of chest width |
| Wide-Chested Dogs (Bulldogs, etc.) | DORSAL recumbency. Start in lateral until intubated, then transition to dorsal. Hands stacked on mid-sternum. | NEW 2024: One-quarter (25 percent) of chest depth to avoid overcompression and rib fractures |
Critical compression parameters:
- Rate: 100 to 120 compressions per minute
- Cycle length: Uninterrupted 2-minute cycles
- Compressor rotation: Rotate compressor every 2 minutes to prevent fatigue
- Full recoil: Allow complete chest wall recoil between compressions
- Minimize interruptions: Hands-off time should be less than 10 seconds per 2-minute cycle
Ventilation
Effective ventilation maintains oxygenation and removes carbon dioxide. The 2024 RECOVER guidelines prioritize bag-mask ventilation over mouth-to-snout for non-intubated patients due to zoonotic disease concerns.
Intubated patients:
- Rate: 10 breaths per minute (one breath every 6 seconds)
- Tidal volume: 10 mL per kg
- Inspiratory time: 1 second
- Oxygen: 100 percent oxygen is reasonable, though room air may also be considered
- Peak airway pressure: 30 to 40 cm H2O if using anesthesia circuit
Non-intubated patients:
- PREFERRED: Tight-fitting mask with manual resuscitator bag. Occlude any vents on mask. Use masks with rubber gaskets for best seal.
- ALTERNATIVE: Mouth-to-snout ventilation ONLY if no zoonotic disease risk. Compression-to-ventilation ratio: 30 compressions to 2 breaths.
- If unsafe: Perform compression-only CPR
Board Tip: The 2024 guidelines updated ventilation recommendations for non-intubated patients. Bag-mask ventilation is now prioritized over mouth-to-snout due to concerns about zoonotic disease transmission (especially relevant post-COVID). This is a change from 2012 guidelines and may appear on NAVLE questions testing knowledge of current best practices.
Advanced Life Support (ALS)
Advanced Life Support encompasses interventions beyond basic CPR, including drug therapy, defibrillation, and treatment of underlying causes. ALS is initiated once BLS is established and additional personnel are available.
Drug Therapy
| Drug | Dose | Indication | Notes |
|---|---|---|---|
| Epinephrine | 0.01 mg per kg IV or IO | BOTH shockable and non-shockable rhythms. Give every 3-5 minutes. | NEW 2024: High-dose epinephrine (0.1 mg per kg) is NO LONGER recommended |
| Vasopressin | 0.8 units per kg IV or IO (single dose) | Alternative vasopressor for refractory VF or pulseless VT | One-time dose only. Potent vasoconstrictor without beta-agonist effects. |
| Atropine | 0.04 mg per kg IV or IO | Asystole or PEA with suspected vagal tone | NEW 2024: Single dose only (not repeated). High doses associated with poor outcomes. |
| Reversal Agents | Naloxone, flumazenil, atipamezole - per drug-specific dosing | CPA secondary to opioid, benzodiazepine, or alpha-2 agonist overdose | Administer if known overdose is cause of CPA |
| Calcium Gluconate | 50 to 100 mg per kg IV slow | Documented hypocalcemia or hyperkalemia | NOT routine. Only if specific indication present. |
| Sodium Bicarbonate | 1 mEq per kg IV | Documented severe metabolic acidosis or prolonged CPR | NOT routine. May worsen intracellular acidosis if given too early. |
Vascular access:
- PREFERRED: Intravenous (IV) catheter if already placed or can be placed within 2 minutes
- ALTERNATIVE: Intraosseous (IO) catheter if IV access not achievable. Sites: proximal humerus, proximal femur, tibial crest
- LEAST PREFERRED: Intratracheal (IT) route for lipophilic drugs only (epinephrine, atropine, naloxone, vasopressin). Dose is 2 to 3 times IV dose.
Memory Tip for 2024 Drug Changes: 'Single and Standard' SINGLE dose of atropine (not repeated like before) STANDARD dose of epinephrine only (NO high-dose anymore) This helps remember the two major 2024 drug changes from the previous guidelines.
Defibrillation
Electrical defibrillation is the ONLY definitive treatment for ventricular fibrillation (VF) and pulseless ventricular tachycardia (VT). The 2024 guidelines emphasize that defibrillation should precede epinephrine administration for shockable rhythms.
Defibrillation protocol:
- Biphasic defibrillator: PREFERRED over monophasic
- Energy dose: 4 to 6 joules per kg for external defibrillation, 0.5 to 1 joule per kg for internal defibrillation
- Single-shock therapy: Deliver one shock, then immediately resume compressions (minimizes interruption)
- If VF/VT less than 4 minutes duration: Immediate defibrillation
- If VF/VT greater than 4 minutes duration: Perform 2-minute BLS cycle FIRST to improve coronary perfusion, THEN defibrillate
Board Tip: A key 2024 update: For shockable rhythms, defibrillation now takes priority over epinephrine administration. The sequence is: Recognize VF/VT → Defibrillate (or BLS for 2 minutes then defibrillate if greater than 4 minutes) → Resume compressions immediately → Give epinephrine. This differs from treating non-shockable rhythms where epinephrine comes first.
Monitoring During CPR
End-Tidal CO2 (ETCO2)
End-tidal CO2 monitoring is the MOST important parameter for assessing CPR quality and detecting return of spontaneous circulation (ROSC). ETCO2 reflects cardiac output and pulmonary blood flow.
ETCO2 targets and interpretation:
- During CPR: Target ETCO2 greater than or equal to 18 mm Hg. Higher values correlate with improved ROSC and survival.
- ETCO2 less than 10 mm Hg: Indicates inadequate compressions. Improve depth, rate, or hand placement.
- Confirming intubation: ETCO2 greater than or equal to 12 mm Hg confirms appropriate endotracheal tube placement (but low ETCO2 does not rule out correct placement).
- Sudden increase in ETCO2: ROSC has occurred. Stop compressions and assess pulse.
Other Monitoring Parameters
- Electrocardiography (ECG): Essential for rhythm diagnosis. Check rhythm only during 2-minute cycle breaks to minimize interruptions.
- Direct blood pressure: Arterial line if available. Target diastolic pressure greater than 20 mm Hg during CPR.
- NOT recommended: Pulse oximetry and arterial blood gases (require pulsatile flow, unreliable during CPR)
Post-Cardiac Arrest Care
The majority of dogs achieving ROSC will either re-arrest or require euthanasia due to post-cardiac arrest syndrome. Approximately 68 percent of dogs experience re-arrest within hours of initial ROSC. Aggressive post-arrest management is essential.
Post-Cardiac Arrest Syndrome
Post-cardiac arrest syndrome consists of four key components:
- Post-cardiac arrest myocardial dysfunction: Transient but significant decrease in contractility
- Post-cardiac arrest brain injury: Anoxic-ischemic injury with potential for delayed neuronal death
- Systemic ischemia-reperfusion response: Systemic inflammatory response syndrome (SIRS), multiorgan dysfunction
- Persistent precipitating pathology: The original cause of CPA (sepsis, trauma, cardiac disease)
Management priorities:
| Parameter | Goals and Interventions |
|---|---|
| Blood Pressure | Target: Mean arterial pressure 80-100 mm Hg, or systolic greater than 100 mm Hg. Treat hypotension with fluids, vasopressors, or inotropes as indicated. |
| Ventilation | Maintain normocarbia. Avoid hyperventilation (worsens cerebral vasoconstriction) and hypoventilation (worsens acidosis). Target ETCO2: 35-45 mm Hg. |
| Oxygenation | Maintain adequate oxygenation but avoid hyperoxia. Target SpO2: 94-98 percent. |
| Temperature | Slow rewarming if hypothermic (less than 1 degree Celsius per hour). Avoid hyperthermia (greater than 39 degrees Celsius). Passive warming preferred. |
| Glucose | Avoid both hypoglycemia (less than 60 mg per dL) and hyperglycemia (greater than 180 mg per dL). Monitor closely. |
| Seizures | Treat seizures aggressively with benzodiazepines (midazolam 0.1-0.3 mg per kg IV) or levetiracetam (30-50 mg per kg IV). |
| Acid-Base | Monitor lactate (normal less than 2 mmol per L). Progressive lactate clearance is favorable. Severe acidosis (pH less than 7.1) may require bicarbonate. |
Prognosis and Prognostic Factors
Survival Statistics
Overall prognosis for CPA in dogs remains poor despite optimal CPR:
- Return of spontaneous circulation (ROSC): 35-58 percent of dogs achieve ROSC
- Survival to discharge: Only 5-7 percent of dogs survive to hospital discharge
- Re-arrest rate: Approximately 68 percent of dogs re-arrest within hours of achieving ROSC
Favorable Prognostic Factors
- Anesthesia-related CPA: 17 times more likely to survive to discharge compared to other causes
- Witnessed arrest with immediate CPR
- Reversible underlying cause (vagal event, drug overdose, airway obstruction)
- Short duration of CPA (less than 5 minutes to ROSC)
- Higher ETCO2 during CPR (greater than 18 mm Hg)
- Cats (5 times more likely to survive than dogs)
- Adherence to RECOVER guidelines (improved ROSC rates demonstrated in studies)
Unfavorable Prognostic Factors
- Advanced neoplasia
- Sepsis
- Severe trauma
- End-stage organ disease
- Prolonged CPR (greater than 10 minutes)
- Low ETCO2 during CPR (less than 10 mm Hg)
- Multiple re-arrest episodes
Memory Tip - Good Prognosis Factors: 'AWARE' Anesthesia-related (best prognosis - 17x better!) Witnessed arrest Acute/reversible cause Rapid ROSC (under 5 minutes) Elevated ETCO2 (greater than 18)
Practice Question
| A 4-year-old male neutered Doberman Pinscher collapses during a routine dental cleaning under general anesthesia. The anesthetist notes that the ECG shows a flat line with no electrical activity. The dog is unresponsive, not breathing, and has no palpable pulse. Chest compressions are initiated immediately at 110 compressions per minute with the dog in lateral recumbency. An endotracheal tube is already in place, and ventilation is provided at 10 breaths per minute with 100 percent oxygen. After 2 minutes of CPR, the ECG still shows asystole and ETCO2 is 8 mm Hg. Which of the following is the MOST appropriate next step? A. Administer epinephrine 0.01 mg per kg IV and continue CPR B. Defibrillate immediately at 4 joules per kg C. Administer atropine 0.04 mg per kg IV and continue CPR D. Increase compression rate to 150 per minute to improve ETCO2 E. Place dog in dorsal recumbency and compress over sternum |
|---|
Correct Answer: A
Explanation
Option A is correct. Asystole is a non-shockable rhythm, and epinephrine is the first-line vasopressor for non-shockable rhythms according to the 2024 RECOVER guidelines. The low ETCO2 of 8 mm Hg (target is greater than or equal to 18 mm Hg) suggests inadequate compressions, so the team should also evaluate compression technique. Epinephrine causes peripheral vasoconstriction, redirecting blood flow to the heart and brain, which is the primary mechanism for improving outcomes in asystole.
Why other options are incorrect:
Option B (Defibrillation) is incorrect because asystole is a non-shockable rhythm. Defibrillation is only indicated for ventricular fibrillation or pulseless ventricular tachycardia. Attempting to defibrillate asystole is not only ineffective but delays appropriate treatment with vasopressors and high-quality CPR.
Option C (Atropine) is partially correct but not the MOST appropriate answer. While atropine may be considered for asystole, especially with suspected vagal tone (which is plausible in this anesthetic case), the 2024 guidelines state that atropine is given as a SINGLE dose and may be considered AFTER epinephrine. Epinephrine remains the priority vasopressor. Additionally, atropine should only be given once during the CPR event.
Option D (Increase compression rate) is incorrect because the current compression rate of 110 per minute is within the recommended range of 100-120 per minute. While the low ETCO2 suggests inadequate compressions, the problem is more likely compression depth, hand placement, or compressor fatigue rather than rate. Increasing rate to 150 per minute exceeds guidelines and may actually worsen chest wall recoil and decrease effectiveness.
Option E (Dorsal recumbency) is incorrect because dorsal recumbency with sternal compressions is reserved for wide-chested dogs (Bulldogs, Boxers) and should only be used after intubation is secured. A Doberman Pinscher is a deep-chested breed that benefits from lateral chest compressions over the widest part of the thorax. Additionally, the dog is already intubated, so there's no contraindication to lateral positioning, which is biomechanically superior for most breeds.
Clinical Pearl: This case highlights the importance of distinguishing shockable from non-shockable rhythms, which determines the entire treatment algorithm. Asystole and PEA require vasopressors and high-quality CPR, while VF and pulseless VT require defibrillation as the priority. The low ETCO2 also emphasizes the value of capnography during CPR - values less than 10 mm Hg indicate that compression quality must be improved immediately (check depth, rate, hand placement, compressor fatigue). Remember that anesthesia-related arrests have much better prognosis (17 times more likely to survive), so aggressive resuscitation is warranted in this case.
Summary and Key Takeaways
- Cardiopulmonary arrest is the cessation of effective cardiac and respiratory function. Recognition must be rapid (within 10-15 seconds) and CPR initiated immediately without checking pulse.
- The 2024 RECOVER guidelines provide evidence-based CPR recommendations including key updates: wide-chested dogs receive 25 percent compression depth in dorsal position, high-dose epinephrine is no longer used, atropine given only once, and bag-mask ventilation preferred over mouth-to-snout.
- Basic Life Support includes high-quality chest compressions at 100-120 per minute in 2-minute uninterrupted cycles with complete recoil, plus ventilation at 10 breaths per minute for intubated patients.
- Advanced Life Support treatment depends on cardiac rhythm: Non-shockable rhythms (asystole, PEA) receive epinephrine every 3-5 minutes; Shockable rhythms (VF, pulseless VT) receive defibrillation as priority.
- ETCO2 monitoring is essential - target greater than or equal to 18 mm Hg during CPR, and sudden increase indicates ROSC. Values less than 10 mm Hg require immediate improvement of compression quality.
- Prognosis is poor overall (5-7 percent survival to discharge), but anesthesia-related arrests have 17 times better survival. Post-cardiac arrest syndrome requires intensive monitoring and aggressive management of hemodynamics, ventilation, temperature, and neurologic function.
- Breed considerations: Small dogs and cats use circumferential compression techniques; medium/large dogs use lateral recumbency with hands over widest chest part; wide-chested dogs may use dorsal recumbency with reduced compression depth.
Image Sources
- RECOVER Initiative - 2024 CPR Algorithm for Dogs and Cats. Available at: https://recoverinitiative.org/2024-algorithms-drug-charts/ (Open access educational resource, no permission required)
- Journal of Veterinary Emergency and Critical Care - CPA Pathophysiology Diagram. Burkitt-Creedon J, et al. 2024 RECOVER Guidelines. J Vet Emerg Crit Care. 2024;34(S1). https://onlinelibrary.wiley.com/doi/10.1111/vec.13391 (Open access journal article)
- https://obgynkey.com/6-the-management-of-cardiac-arrest/
- Today's Veterinary Practice - ECG Rhythm Examples. CPR for Dogs and Cats: The RECOVER Guidelines. February 2022. https://todaysveterinarypractice.com/emergency-medicine-critical-care/cardiopulmonary-resuscitation-the-recover-guidelines/ (Open access educational content)
- Cornell University College of Veterinary Medicine - Pet CPR Infographic showing chest compression hand placement. Available at: https://www.vet.cornell.edu/about-us/news/pet-cpr-infographic-just-released (Free educational resource for public use)
- Journal of Veterinary Emergency and Critical Care - Chest Compression Technique Illustrations by Allison Buck. From: Hopper K, et al. 2024 RECOVER Guidelines: Basic Life Support. J Vet Emerg Crit Care. 2024;34(S1):16-43. https://onlinelibrary.wiley.com/doi/10.1111/vec.13387 (Open access journal article with educational illustrations)
- Merck Veterinary Manual - Defibrillation Technique in Small Animals. https://www.merckvetmanual.com/emergency-medicine-and-critical-care/specific-diagnostics-and-therapy/cardiopulmonary-resuscitation-of-small-animals (Open access veterinary reference)
References
- Burkitt-Creedon JM, Hopper K, Epstein SE, et al. 2024 RECOVER Guidelines: Updated treatment recommendations for CPR in dogs and cats. J Vet Emerg Crit Care. 2024;34(S1):4-15. doi:10.1111/vec.13391
- Hopper K, Epstein SE, Burkitt-Creedon JM, et al. 2024 RECOVER Guidelines: Basic Life Support. Evidence and knowledge gap analysis with treatment recommendations for small animal CPR. J Vet Emerg Crit Care. 2024;34(S1):16-43. doi:10.1111/vec.13387
- Fletcher DJ, Boller M, Brainard BM, et al. RECOVER evidence and knowledge gap analysis on veterinary CPR. Part 7: Clinical guidelines. J Vet Emerg Crit Care. 2012;22(S1):S102-S131.
- Hoehne SN, Hopper K, Epstein SE. Prospective evaluation of cardiopulmonary resuscitation performed in dogs and cats according to the RECOVER Guidelines. Part 2: patient outcomes and CPR practice since guideline implementation. Front Vet Sci. 2019;6:439. doi:10.3389/fvets.2019.00439
- Kawase K, Ujiie H, Takaki M, Yamashita K. Clinical outcome of canine cardiopulmonary resuscitation following the RECOVER clinical guidelines at a Japanese nighttime animal hospital. J Vet Med Sci. 2018;80(3):518-525. doi:10.1292/jvms.17-0107
- Dazio VER, Gay JM, Hoehne SN. Cardiopulmonary resuscitation outcomes of dogs and cats at a veterinary teaching hospital before and after publication of the RECOVER guidelines. J Small Anim Pract. 2023;64(4):270-279. doi:10.1111/jsap.13582
- Hofmeister EH, Brainard BM, Egger CM, Kang S. Prognostic indicators for dogs and cats with cardiopulmonary arrest treated by cardiopulmonary cerebral resuscitation at a university teaching hospital. J Am Vet Med Assoc. 2009;235(1):50-57.
- Cardiopulmonary Resuscitation of Small Animals. Merck Veterinary Manual. Accessed December 2024. https://www.merckvetmanual.com/emergency-medicine-and-critical-care/specific-diagnostics-and-therapy/cardiopulmonary-resuscitation-of-small-animals
- Boller M, Boller EM, Oodegard S, Otto CM. Small animal cardiopulmonary resuscitation requires a continuum of care: proposal for a chain of survival for veterinary patients. J Am Vet Med Assoc. 2012;240(5):540-554.
- Plunkett SJ, McMichael M. Cardiopulmonary Arrest & Life Support. Clinician's Brief. April 2008. https://www.cliniciansbrief.com/columns/42/cardopulmonary-arrest-life-support
Practice NAVLE Questions
Test your knowledge with 10,000+ exam-style questions, detailed explanations, and timed exams.
Start Your Free Trial →